Effect of Spinal Manipulation in Piriformis Syndrome. A case study
ABSTRACT
Objective: The objective of this study is to describe the efficacy of spinal manipulation therapy in the clinical management of a patient with sciatica symptoms due to piriformis syndrome. This is a condition which can be overlooked or misdiagnosed easily.
Clinical features: A 35-year-old male patient is presented with chronic pain over the right lower back and a gluteal region which becomes worse with prolonged sitting. Physical examination showed reduced and painful lumbar movement on combined extension, right side rotation, and right side bending. Right buttock pain was increased on flexion, adduction and internal rotation of the right hip.
Intervention and outcome: A high-velocity low-amplitude thrust (HVLAT) spinal manipulation was used as a primary treatment along with muscle stretching, strengthening and neuromuscular training exercise as a home exercise program. The patient received 3 treatments over a period of 4 weeks. Long term effect could not be evaluated.
Conclusion: Spinal manipulative therapy can be used to treat the effect and possibly the cause of piriformis syndrome. Further, studies are warranted.
INTRODUCTION
Piriformis syndrome (PS) is a peripheral neuritis of the sciatic nerve caused by the compression of nerve trunk due to or related to, the excessive contraction, spasm, injury or inflammation of the piriformis muscle (Windisch & Braun, 2007; Cummings, 2000; Parziale, Hudgins & Fishman, 1996). Piriformis syndrome is frequently overlooked or misdiagnosed as it can mimic other common somatic dysfunctions such as sacroiliac (SI) dysfunctions, lumbar facet joint dysfunctions, sciatica, herniated intervertebral disc, etc (O’Neill, McClain, Coleman & Thomas, 2008).
Piriformis syndrome is generally characterized by pain in the buttock, hips and lower limbs which worsen after sitting for longer than 15-20 minutes (Papadopoulos & Khan, 2004; Foster, 2002; Parziale et. al., 1996). Chronicity of PS may lead to pathologic conditions of the sciatic nerve, other surrounding nerves and vessels, chronic somatic dysfunctions, which eventually results in chronic radiating pain, paresthesia, hyperesthesia and muscle weakness (Chaitlow, 1988 as cited in O’Neill et al., 2008). Delay in addressing PS may lead to compensatory or facilitative changes which can contribute to cervical, thoracic and lumbosacral dysfunctions and pain (Steiner, Staubs, Ganon & Buhlinger, 1987; TePoorten, 1969).
Piriformis syndrome is common during the fourth and fifth decades of life regardless of activity levels or occupations (Beaton & Anson, 2008; Foster, 2002; Beaty, 1994). PS is reported from 5% to 36% among patients with low back pain (Foster, 2002). Filler et al., (2005) have reported 67% of non-disc sciatic pain is related to PS. However, it is surprising to see that apart from a few case reports and systemic reviews, PS has received very little attention in the research field.
Various etiological factors for PS have been described in literature such as gluteal trauma, anatomical variants as double piriformis, myofascial trigger points, hypertrophy and spasm of piriformis muscle, SI dysfunction, lumbar hyperlordosis, lower limb dissymmetry and other biomechanical alterations ( Jankovic, Peng & Zundert, 2013; Ruiz, Alfonso & Villalon, 2008. However, the presentation of significantly identifiable cause is not seen in most patients (Jankovic, 2013). Physical assessment of PS should include a structural or mechanical examination of lumbar, pelvis and sacrum (Retzlaff, 1974 as cited in O’Neill et al., 2008; TePoorten, 1969). SI joint function and other biomechanical alterations should be considered as possible causes or effects during the assessment, diagnosis and treatment of piriformis syndrome (Papadopoulos et al., 2004; Benzon, Katz, Benzon & Iqbal, 2003; Benson & Schutzer, 1999; Steiner et al., 1987).
The aim of this study is to evaluate the effect of high-velocity low-amplitude thrust (HVLAT) manipulation in the treatment of piriformis syndrome along with other traditional physical therapy approaches such as stretching and strengthening exercises.
CASE REPORT
History:
The patient was a 35-year-old male, working as a chef from the last 15 months and as a gardener before. He presented with a 3 months history of increasing pain in right lower back and buttock pain with occasional radiating pain down the posterior thigh. From last 3 weeks, pain is getting worse and has started to feel groin pain, pain in the anterior, lateral and posterior thigh. Pain gets worse on sitting for longer than 10-15 minutes and has to change his sitting position frequently. Also, he is feeling slight numbness along the posterolateral thigh up to the mid-calf region on prolonged sitting. He reported 3/10 pain in VAS scale at best which goes up to 7/10 during prolong sitting and during his work. The pain is disturbing his workability as he frequently needs to sit and stand, stoop forward and lift objects when working in a kitchen. The only pain easing factor was deep overpressure in the groin region. He has a history of recurrent low back pain from last 5 years and has fractured right ankle in his teenage.
Physical examination:
Examination of the lumbar spine revealed a reduced range of motion and pain on combined extension, right side rotation, and right side bend. He was tender on the right L4 and L5 spinous processes, slightly tender, and stiffness on right sacroiliac joint. However, pain provoking tests for SI dysfunctions were negative. Neurological examinations were normal. Slump tests, straight leg raising test, and Valsalva maneuver were negative.
All the diagnostic tests for possible hip conditions were negative. On examination of right gluteal regions revealed diffused tenderness on gluteal muscles with the tenderest point on the myofascial trigger point of the right piriformis muscle. Right piriformis muscle was tighter than the left. Similarly, there was tight muscle band of right side lumbar extensors and right psoas compared to the left side. Various provoking tests for PS were positive such as Lasegues sign (FAIR test – flexion, adduction, internal rotation of the hip); Pace’s sign; Piriformis line test and Beathy’s maneuver.
On strength examination, the patient was weak on hip abduction (4/5) and external rotation (3/5) and hip flexion (3/5). On single leg stance observation, he was imbalanced on the right leg compared to stance on left leg. There was slight atrophy of right gluteal muscles.
Treatment:
First visit:
Left side-lying, rotational, HVLAT manipulation on right L5 – S1. Chicago manipulation for right SI joint. Right side psoas muscle stretch and release.
Outcome: There was a significant increase in the range of motion with reduced pain on the extension, right side rotation and side bend. There was a remarkable reduction in the tightness or tenderness of lumbar extensors and psoas muscles. The patient showed significant improvement in hip flexion strength (4+/5).
Second visit:
The patient came back after one day with much reduced low back pain (2/10) and pain around the hip and posterior thigh (3/10). He can sit for a longer period and be very comfortable at work. He reported no numbness after the first session. Physical examination revealed reduced stiffness on right L4-L5, L5-S1 joint mobility and no pain and stiffness on right SI joint. Reduced pain on piriformis line and Lasegues tests.
Treatment: Left side-lying, rotational, HVLAT manipulation on right L4-L5 and L5-S1. Right piriformis muscle stretch and release. A home exercise program with piriformis stretchings and neuromuscular training for the lower limb to focus on gluteal muscle engagement.
Outcome: The patient reported significant improvement in terms of his low back pain and right side buttock, groin and around the thigh (1/10). There was a remarkable improvement in lower lumbar spine mobility.
Third visit:
The patient came back with no pain. He can sit and work for a long period without any pain. He feels more stable and flexible at work.
The patient was discharged with home exercise programs to continue for three weeks;
– lumbar rotational and side bending exercises to maintain joint mobility.
-piriformis stretchings
-gluteal muscle strengthening exercise.
-neuromuscular training to maintain optimal posterior chain neurodynamics.
DISCUSSION
This case report has demonstrated the significance of therapeutic effectiveness of spinal manipulation to eliminate the pain and possibly the underlying cause of piriformis syndrome.
A various important differential diagnosis such as lumbar disc herniation, sacroiliac joint syndrome and pain due to hip conditions were cleared before interpreting the condition as PS. The possible lumbar disc herniation was eliminated as there were no peripheral neurological symptoms and negative results for slump test, straight leg raising test and Valsalva maneuver (Majlesi, Togay, Unalan & Toprak. 2008; Souza, 2005 as cited in Mayrand, Fortin, Descarreaux & Normand, 2006). Although there were sacroiliac tenderness and mild stiffness compared to the normal side, the possibility of sciatica symptoms due to strain or subluxation of SI joint was minimum. There was no pain when the patient stood up from sitting position and during passive physiological rotations of the pelvis (Souza, 2005 as cited in Mayrand et al., 2006). Also, Gaenslen’s, and Yeoman’s test were negative. Similarly, there was no history of mechanical injury to the hip and no pain with passive physiological movements of the hip joint. So, pain due to any possible hip conditions was excluded.
The aim of the treatment was to reduce pain and numbness, reduce muscle tightness and improve lumbar and sacroiliac joint mobility. Rotational spinal manipulation (HVLAT) inside posture for lumbar and sacroiliac joint were used as the first line of treatment to meet the treatment goals. Piriformis stretching, gluteal strengthening, and neuromuscular training exercises were added into the treatment program and as a home exercise program.
Piriformis syndrome has been shown associated with various degrees of biomechanical alterations mainly in lower lumbar vertebrae and sacroiliac joint. Retzlaff, 1974 (as cited in O’Neill et al., 2008) have reported that piriformis syndrome may lead to anterior rotation of sacrum towards the ipsilateral side on a contralateral axis and compensatory rotation of lower lumbar vertebrae in opposite direction. Pain on combined extension, right rotation, and right side bending and tenderness to the right side of L5 spinous process, in this case, lead us to hypothesize the left-on-left forward sacral torsion with L5 rotated to right.
Spinal manipulation can correct alterations in the normal anatomical, physiological or biomechanical dynamics of the vertebral column and thereby can elicit the normal neuromusculoskeletal system (Picker, 2002). Spinal manipulation can restore Zygapophyseal joint mobility resulting in pain-free motion of the musculoskeletal system (Whittingham & Nilson, 2001). The patient in this study responded well to spinal manipulation (L4-L5, L5-S1). This may be due to the restoration of buckled lower lumbar segment which can reduce mechanical stress or strain on paraspinal tissues or muscles (Triano, 2001 as cited in Picker, 2002). The significant effect on this patient after the first session of treatment might also be due to the improved neurophysiological functions evoked by the changes in the inflow of sensory signals from paraspinal tissues following spinal manipulation (Pickar, 2002).
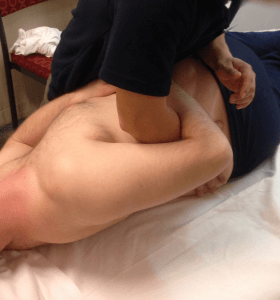
Fig. 1: Side lying, rotational HVLAT spinal manipulation
Spinal manipulation may have both inhibitory and excitatory effects on somatomotor activity (Pickar, 2002). Spinal manipulation has a stretching effect on paraspinal muscle and psoas muscle on the contralateral side and relaxes on the same side of manipulation (Maigne & Vautravers, 2003). Stretching of psoas muscle activates Ib fibres which induce presynaptic inhibition of afferent Ia fibres of agonists (Maigne & Vautravers, 2003) and hence reduction of lumbar extensor muscles activity as in this case. This mechanism may explain the reason for the patient in the study getting ease of pain on deep overpressure in the groin (i.e. may be pressing on psoas muscle). This stretching may be enhanced further by the separation of facet joints and vertebrae induced by spinal manipulation by inhibiting motor unit action potential of paraspinal muscles (Cramer, Tuck & Knudsen, 2000; Bogduk & Jull, 1985). Sacroiliac or lumbar spinal manipulation can reduce H-reflex (Dishman & Bulbulian, 2000). So, spinal manipulation may inhibit H-reflex of nerve to piriformis muscle which can cause attenuation of alpha motor neuron activity of piriformis muscle and hence reducing muscle spasm (Herzog, Scheele & Conway, 1999; Murphy, Dawson & Slack, 1995).
The patient showed improved hip abduction and external rotation strength. This may be explained by the association of spinal manipulation with an increase in muscle strength either through facilitation or disinhibition of neural pathways (Pickar, 2002). Suter, McMorland, Herzog & Bray, (2003) have reported a significant decrease in motor inhibition of knee extensor in symptomatic patients with sacroiliac joint dysfunction following a spinal manipulation.
We found significant improvement with pain-free lumbar movement after the second session of manipulation. This may be due to the release of entrapped synovial folds or intra-articular adhesions that limit motion (Indahl, Kaigle, Reikeras & Holm, 1997).
The patient in this study has a history of recurrent low back pain. Brumagne, Lysens, Swinnen & Verschueren, (1999) have observed weaker or impaired lumbosacral repositioning ability in individuals with the history of low back pain. This may be the cause of overuse of the piriformis muscle, in this case, to compensate for the impaired positioning of the pelvis and lumbosacral spine. Also his nature of work requiring repetitive squat-stand movement, weaker gluteal muscle strength may have enhanced the overuse of piriformis muscle. Spinal manipulation improves paraspinal proprioceptive input thereby resulting in normal optimal positioning of the pelvis and lumbosacral spine (Pickar, 2002). Thus, spinal manipulation may have corrected the cause of piriformis syndrome in this study rather than only reducing local pain and improving pain-free range of motion.
The immediate and significant effect of spinal manipulation seen in this case study was in line with the positive response to manipulative therapy shown by the patients with piriformis syndrome in previous case studies (O;Neill et al., 2008; Maryand et al., 2006; Nancy, 2003). But unlike these studies, we used manipulation as the first line of treatment followed by the exercise training. However, this study could not explain the long term effect of manipulation as it was a short period of study for 4 weeks.
CONCLUSION
High-velocity low amplitude thrust spinal manipulation can be used as an effective technique along with traditional stretching and strengthening exercises to enhance the conservative management of piriformis syndrome. Further, studies in terms of large scale standard intervention and randomized controlled trial studies are warranted to support the findings with scientific evidence.
Reference


Awesome post Thanks for sharing.
Wonderful Blogpost thank you for sharing.
Wonderful post thank you for sharing.
What’s up,I read your blogs named “back pain, piriformis syndrome, sciatica, back pain, spinal manipulation” daily.Your writing style is witty, keep up the good work! And you can look our website about الاهلى.
back pain, piriformis syndrome, sciatica, back pain, spinal manipulation
atpyixixb
tpyixixb http://www.gw2gi6934r136x00hx1ae59j6tzc5gu4s.org/
[url=http://www.gw2gi6934r136x00hx1ae59j6tzc5gu4s.org/]utpyixixb[/url]
Attractive component of content. I just stumbled upon your site and in accession capital to assert that I acquire in fact enjoyed account your weblog posts. Any way I will be subscribing on your feeds and even I fulfillment you access constantly quickly.
thank you. keep visiting the site and appreciate your continuous feedback
Hi! I’m at work browsing your blog from my new iphone 4! Just wanted to say I love reading your blog and look forward to all your posts! Keep up the fantastic work!